Running and Patellofemoral Pain Syndrome: What makes you weak at the knees?
Patellofemoral Pain Syndrome (PFPS) is a knee condition associated with anterior knee pain when loading the knee in movements like squatting, stair climbing, running and jumping (Ferber et al., 2015). Due to its high prevalence and running becoming an increasingly common form of exercise, it is important that high quality evidence regarding treatment and preventative strategies are made accessible to the public.
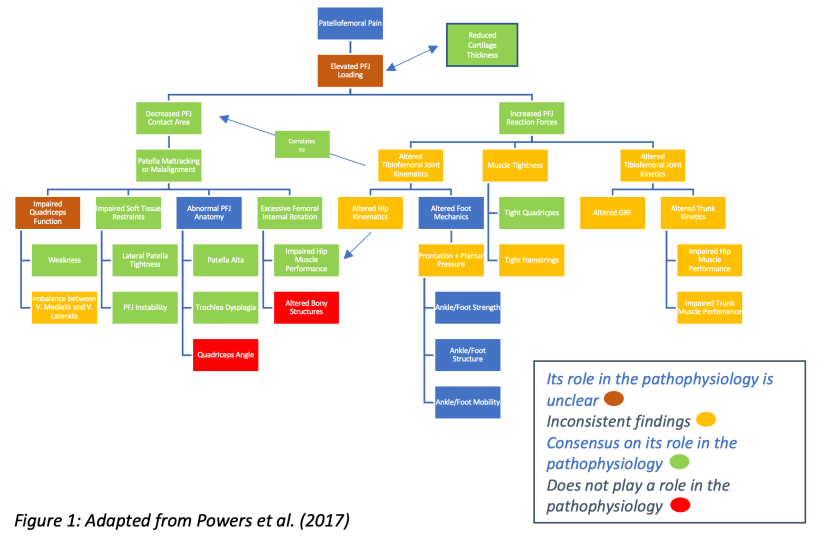
Like most soft tissue injuries, PFPS is also a multifactorial condition involving structural, sensorimotor, somatosensory, psychological, and nociceptive processing changes (Powers et al., 2017). Consequently, a consensus paper was written which outlined the current evidence-based understanding of the complex aetiology of this condition. Figure 1 shows the varied levels of scientific knowledge on the proposed mechanisms of the pathophysiology in PFPS.
To understand how best to deal with PFPS we are going to look at a question posed by Ferber et al.: what is the best form of exercise when treating PFPS? According to the most recent consensus statement on treatment regarding PFPS, there is an understanding that exercise and multimodal treatment involving knee, hip and core training is the most evidence-based approach when treating PFPS (Crossley et al., 2016). However, until 2015, there had not been research into whether, in isolation, a hip and core or knee protocol is more efficient (Feber et al., 2015).
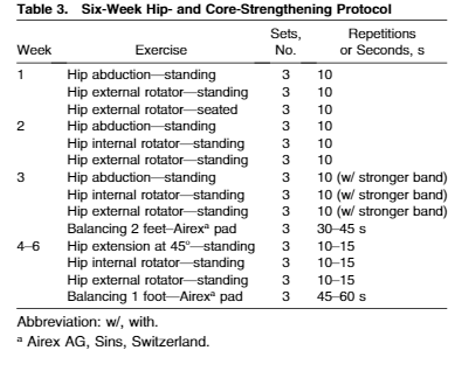
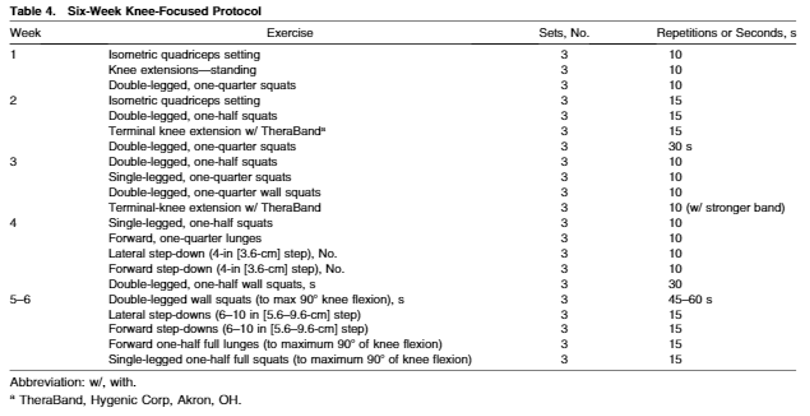
Feber et al. (2015) included 199 individuals suffering from PFPS in the USA in a randomised control trial comparing a 6-week knee protocol (Figure 3) to a 6-week hip and core protocol (Figure 2). These programs used functional exercises to progressively overload the participants throughout the 6-weeks. Both protocols produced similar statistically significant increases in maximum isometric knee extension strength (Hip/Core – 8.04% (p<0.05); Knee – 6.37% (p<0.05)) and functional capacity measured by the Anterior Knee Pain Score (Hip/Core – 12.58% (p<0.05); Knee – 12.90% (p<0.05)) post treatment . However, the hip and core protocol had a greater reduction in VAS pain scores after 3-weeks (p<0.05) even though pain scores were equal at 6 weeks. The hip and core also produced greater hip extension (Hip/Core – 11.34%; Knee – 7.13%; p<0.05) and abduction (Hip/Core – 11.46%; Knee – 8.21%; p<0.05) maximal isometric strength post treatment (Feber et al., 2015). Both of these variables are shown to be possible risk factors for PFPS (Figure 1). Therefore, the hip and core protocol may have a greater efficiency when treating PFPS as it targets more risk factors than the knee protocol.
Therefore, this hip and core exercise protocol, which is time efficient and uses a shotgun approach against the risk factors relating to PFPS, may be a much sort after injury prevention program for runners wanting to avoid future anterior knee pain.
References
Crossley, K. M. et al. (2016) ‘2016 Patellofemoral pain consensus statement from the 4th International Patellofemoral Pain Research Retreat, Manchester. Part 2: Recommended physical interventions (exercise, taping, bracing, foot orthoses and combined interventions)’, British Journal of Sports Medicine, 50(14), pp. 844–852. doi: 10.1136/bjsports-2016-096268.
Ferber, R. et al. (2015) ‘Strengthening of the hip and core versus knee muscles for the treatment of patellofemoral pain: A multicenter randomized controlled trial’, Journal of Athletic Training, 50(4), pp. 366–377. doi: 10.4085/1062-6050-49.3.70.
Powers, C. M. et al. (2017) ‘Evidence-based framework for a pathomechanical model of patellofemoral pain: 2017 patellofemoral pain consensus statement from the 4th International Patellofemoral Pain Research Retreat, Manchester, UK: Part 3’, British Journal of Sports Medicine, 51(24), pp. 1713–1723. doi: 10.1136/bjsports-2017-098717.
One comment